Ambetter Health Topics & 100 FAQs
Ambetter Insurance Basics
Learn how Ambetter health insurance works, including plan types, provider networks, and the medical services typically covered under Ambetter Marketplace plans.
Ambetter Coverage & Benefits
Explore Ambetter Health plans and the Nationwide network, including preventive care, doctor visits, hospital services, prescriptions, and other healthcare benefits.
Understand how to enroll with Ambetter Health for health insurance, including open enrollment periods, qualifying life events, and eligibility requirements.
Understanding Ambetter Health Insurance
Ambetter Health Insurance is a Marketplace health insurance program offered through Centene Corporation and its affiliated health plans in many states across the United States. Ambetter plans are designed to provide comprehensive medical coverage, including doctor visits, hospital care, preventive services, and prescription medications. These plans are typically available through the Health Insurance Marketplace and are structured to meet Affordable Care Act coverage requirements. Understanding how Ambetter plans work, what services may be covered, and how provider networks operate can help individuals choose coverage that fits their healthcare needs. To learn more about Ambetter plan options and coverage details, you can explore Ambetter health insurance plans.
FAQ's
1. What is Ambetter health insurance?
What is Ambetter health insurance?
Ambetter health insurance is a health coverage program offered through Centene Corporation and its affiliated health plans in many states across the United States. Ambetter plans are typically available through the Health Insurance Marketplace and are designed to meet Affordable Care Act (ACA) coverage requirements.
These plans help individuals and families access essential medical services such as doctor visits, hospital care, preventive screenings, and prescription medications. Coverage options may vary by state and by the specific Ambetter health plan available in that region.
Individuals who want to learn more about available coverage options can review Ambetter health insurance plans to better understand how these policies work.
2. Who offers Ambetter health insurance?
Who offers Ambetter health insurance?
Ambetter health insurance is offered through Centene Corporation, a healthcare company that works with state-based health plans across the United States. Through these affiliated health plans, Ambetter provides Marketplace coverage that meets Affordable Care Act guidelines.
Because Ambetter operates through regional health plans, the exact provider networks, coverage options, and plan details may vary depending on the state where coverage is offered.
Individuals can explore health insurance options available by state to better understand which plans and provider networks are available in their location.
3. What type of health insurance plans does Ambetter offer?
What type of health insurance plans does Ambetter offer?
Ambetter primarily offers Affordable Care Act Marketplace health insurance plans designed to provide comprehensive medical coverage. These plans include coverage for essential health services such as preventive care, hospital services, prescription medications, and doctor visits.
Ambetter plans are typically organized into different coverage tiers that balance monthly premiums with cost-sharing structures such as deductibles, copays, and coinsurance. These options allow individuals to choose plans that fit their healthcare needs and budget preferences.
Learning how different coverage tiers work can help individuals compare plan options more effectively.
4. What states offer Ambetter health insurance?
What states offer Ambetter health insurance?
Ambetter health insurance is available in many states across the United States, although the specific plans and provider networks offered may vary depending on the region. Because healthcare providers and insurance regulations differ between states, coverage options are often tailored to the local healthcare system.
Individuals interested in learning which plans are available in their area can review health insurance plans by state to explore coverage options offered where they live.
5. What services are typically covered by Ambetter plans?
What services are typically covered by Ambetter plans?
Ambetter health insurance plans generally cover a wide range of medical services that meet Affordable Care Act requirements. These services often include preventive care visits, primary care appointments, hospital care, prescription medications, mental health services, and emergency treatment.
Preventive care services may include routine checkups, screenings, and vaccinations designed to help detect health concerns early and maintain overall wellness.
Coverage details may vary depending on the specific plan selected and the provider network associated with that policy.
6. How do Ambetter provider networks work?
How do Ambetter provider networks work?
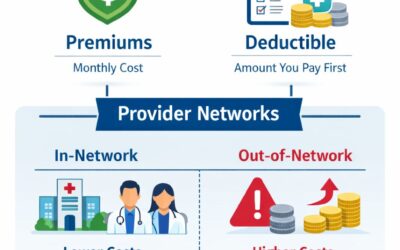
Ambetter health insurance plans use provider networks that include doctors, hospitals, clinics, and healthcare facilities that have agreements with the insurance company to provide services at negotiated rates. These networks help control healthcare costs while ensuring members have access to medical providers.
When members receive care from providers within the network, they typically benefit from lower healthcare costs because the negotiated pricing agreements apply to covered services.
Understanding how provider networks operate can help individuals select plans that include their preferred doctors and healthcare facilities.
7. Does Ambetter cover preventive healthcare services?
Does Ambetter cover preventive healthcare services?
Ambetter health insurance plans generally include preventive healthcare services designed to help detect health concerns early and support long-term wellness. Preventive services may include routine checkups, vaccinations, screenings, and other health evaluations recommended by medical professionals.
These services play an important role in maintaining overall health and may help identify potential medical conditions before they become more serious health issues.
8. How does Ambetter health insurance differ from other insurance companies?
How does Ambetter health insurance differ from other insurance companies?
Ambetter health insurance operates through regional health plans that participate in the Health Insurance Marketplace. Because of this structure, Ambetter plans are often designed specifically for Marketplace consumers seeking comprehensive medical coverage.
Each insurance company may structure its provider networks, coverage options, and cost-sharing features differently. Individuals comparing carriers may find it helpful to review resources such as UnitedHealthcare FAQs or Oscar Health FAQs to better understand how different insurers organize their plans.
9. Can individuals choose their doctors with Ambetter plans?
Where can someone learn more about Ambetter health insurance?
Individuals interested in learning more about Ambetter health insurance can review educational resources that explain plan structures, provider networks, and enrollment options. Understanding how coverage works can help individuals make informed decisions when selecting health insurance.
Additional information about coverage options and plan details can be found by exploring Ambetter health insurance plans and other educational resources available through the Vivna health insurance blog.
10. Where can someone learn more about Ambetter health insurance?
Where can someone learn more about Ambetter health insurance?
Individuals interested in learning more about Ambetter health insurance can review educational resources that explain plan structures, provider networks, and enrollment options. Understanding how coverage works can help individuals make informed decisions when selecting health insurance.
Additional information about coverage options and plan details can be found by exploring Ambetter health insurance plans and other educational resources available through the Vivna health insurance blog.
11. Is Ambetter health insurance part of the Health Insurance Marketplace?
Is Ambetter health insurance part of the Health Insurance Marketplace?
Yes, Ambetter health insurance plans are commonly offered through the Health Insurance Marketplace established under the Affordable Care Act. Marketplace plans are designed to provide comprehensive medical coverage that meets federal healthcare standards for essential health benefits. These benefits typically include preventive care, doctor visits, hospital services, prescription medications, mental health care, and other important healthcare services.
Marketplace plans allow individuals and families to compare coverage options from different insurance carriers in one place. Because Ambetter participates in many state marketplaces, individuals may be able to review multiple Ambetter plan options depending on where they live. These plans are structured to provide standardized coverage while allowing consumers to select a policy that aligns with their healthcare needs and budget.
Individuals interested in learning more about Marketplace coverage can explore open enrollment health insurance information to better understand when enrollment opportunities are available and how Marketplace plans work.
12. Does Ambetter health insurance meet Affordable Care Act requirements?
Does Ambetter health insurance meet Affordable Care Act requirements?
Ambetter health insurance plans are designed to meet the coverage standards established by the Affordable Care Act. These standards require health insurance policies to provide a set of essential health benefits that help ensure individuals have access to comprehensive medical care. Essential health benefits typically include preventive care services, emergency care, hospital treatment, maternity care, prescription medications, and mental health services.
Another important feature of ACA-compliant plans is that coverage cannot be denied due to pre-existing medical conditions. This rule ensures that individuals can obtain health insurance regardless of their past health history. Ambetter plans also follow regulations that protect consumers by limiting certain types of coverage restrictions and requiring clear explanations of benefits.
Understanding how ACA-compliant plans work can help individuals compare coverage options and determine whether Marketplace coverage meets their healthcare needs.
13. How does Ambetter health insurance help individuals access healthcare?
How does Ambetter health insurance help individuals access healthcare?
Ambetter health insurance helps individuals access healthcare by connecting members with networks of physicians, hospitals, clinics, and healthcare providers that participate in the insurance plan. These provider networks allow patients to receive medical services at negotiated rates, which helps reduce the overall cost of care.
Members may use their insurance coverage to schedule appointments with doctors, obtain preventive care, receive hospital treatment, and access prescription medications according to the coverage rules of their policy. Having health insurance also helps individuals manage healthcare expenses by sharing the cost of medical services between the insurance provider and the policyholder.
Learning how provider networks and insurance coverage work together can help individuals better navigate the healthcare system and obtain necessary medical care when it is needed.
14. What types of medical providers participate in Ambetter networks?
What types of medical providers participate in Ambetter networks?
Ambetter health insurance networks typically include a variety of healthcare providers such as primary care physicians, medical specialists, hospitals, urgent care centers, diagnostic facilities, and pharmacies. These providers work with the insurance company to deliver medical services to members at negotiated rates.
Provider networks help coordinate healthcare services and ensure that patients have access to medical professionals who are familiar with the coverage rules of the insurance plan. Because each network is built around regional healthcare systems, the available providers may vary depending on the state where coverage is offered.
Individuals can review provider directories to confirm whether specific doctors or hospitals participate in the Ambetter network before scheduling appointments.
15. Does Ambetter health insurance include preventive care?
Does Ambetter health insurance include preventive care?
Ambetter health insurance plans generally include preventive healthcare services designed to help detect medical conditions early and support long-term health. Preventive services may include routine wellness visits, health screenings, immunizations, and other medical evaluations recommended by healthcare professionals.
Preventive care plays an important role in maintaining overall health because it allows doctors to identify potential health concerns before they become serious conditions. Early detection can lead to better treatment outcomes and help individuals manage their health more effectively.
Many comprehensive health insurance plans include preventive services as part of their standard coverage benefits, although specific services may vary depending on the plan structure.
16. How do members use Ambetter health insurance after enrolling?
How do members use Ambetter health insurance after enrolling?
Once enrolled in an Ambetter health insurance plan, members typically receive an insurance identification card that can be presented when visiting doctors, hospitals, or pharmacies. Healthcare providers use this information to verify coverage and submit claims to the insurance company for services provided.
Members may schedule appointments with in-network healthcare providers and receive medical services according to the coverage rules of their policy. The insurance company then processes claims and determines how costs are shared between the provider, the insurer, and the patient.
Understanding how to use health insurance effectively can help individuals access care more easily and avoid confusion when receiving medical services.
17. How can someone determine if Ambetter is available in their state?
How can someone determine if Ambetter is available in their state?
Ambetter health insurance plans are available in many states across the United States, although plan availability and provider networks may vary depending on regional healthcare systems. Because insurance companies work with local providers and state regulations, coverage options may differ from one state to another.
Individuals who want to review health insurance options available in their region can explore health insurance plans by state. Reviewing state-specific information can help individuals understand which insurance carriers operate in their area and what types of coverage may be available.
This information can be helpful when comparing insurance providers and selecting a plan that offers access to preferred doctors and healthcare facilities.
18. Are Ambetter plans available to individuals and families?
Are Ambetter plans available to individuals and families?
Ambetter health insurance plans are typically available to both individuals and families seeking comprehensive medical coverage through the Health Insurance Marketplace. These plans are designed to help provide access to healthcare services for people who may not receive insurance through an employer.
Individuals can compare different plan options to determine which coverage structure best fits their household healthcare needs. Family coverage may include benefits for multiple household members under a single policy, helping ensure consistent access to healthcare services.
Reviewing plan details carefully can help individuals determine whether a particular policy offers the provider access and coverage features that best meet their needs.
19. How does Ambetter compare to other insurance carriers?
How does Ambetter compare to other insurance carriers?
Ambetter is one of several health insurance providers that participate in Marketplace coverage programs. Each insurance carrier structures its plans differently based on provider networks, coverage features, and cost-sharing models such as deductibles and copays.
Because different carriers negotiate separate agreements with hospitals and doctors, provider networks and coverage structures may vary between insurers. Individuals often compare multiple carriers to determine which plan offers the best combination of provider access and healthcare benefits.
To better understand how different insurance companies structure their plans, individuals may review resources such as UnitedHealthcare FAQs, Oscar Health FAQs, or Molina Healthcare FAQs.
20. Where can someone learn more about Ambetter health insurance plans?
Where can someone learn more about Ambetter health insurance plans?
Individuals who want to learn more about Ambetter health insurance can review educational resources that explain plan structures, coverage benefits, and enrollment opportunities. Understanding how health insurance works can help individuals make more informed decisions when selecting coverage.
Additional information about Ambetter plan options and provider networks can be found by exploring Ambetter health insurance plans. Educational resources such as the Vivna health insurance blog may also provide helpful insights into how health insurance coverage works.
Learning more about insurance coverage helps individuals navigate the healthcare system with greater confidence and access medical care more effectively.
Understanding Ambetter Health Insurance Costs
Ambetter health insurance plans use a cost-sharing structure that includes monthly premiums, deductibles, copays, and coinsurance. These elements work together to determine how healthcare expenses are divided between the insurance provider and the policyholder. Marketplace plans offered through Ambetter are designed to balance coverage with affordability by offering multiple plan tiers with different premium levels and cost-sharing structures. Understanding how these costs work can help individuals compare plans more effectively and choose coverage that aligns with their healthcare needs and financial situation. Individuals interested in learning more about Marketplace enrollment and cost assistance programs can review open enrollment health insurance information to better understand how Marketplace coverage works.
FAQ's
21. What is the monthly premium for an Ambetter health insurance plan?
What is the monthly premium for an Ambetter health insurance plan?
The monthly premium is the amount a policyholder pays each month to maintain active health insurance coverage. Ambetter health insurance plans offer different premium levels depending on the plan tier selected, the region where the coverage is offered, and other factors such as age and household composition.
Plans with lower monthly premiums may have higher deductibles or cost sharing, while plans with higher monthly premiums may offer lower out-of-pocket costs when medical services are used. Because Ambetter plans are offered through the Health Insurance Marketplace, individuals may have access to financial assistance programs that can help reduce monthly premium costs.
Understanding how premiums work can help individuals compare health insurance plans and select coverage that fits their budget and healthcare needs.
22. What is a deductible in an Ambetter health insurance plan?
What is a deductible in an Ambetter health insurance plan?
A deductible is the amount a policyholder must pay for covered medical services before the insurance plan begins sharing the cost of care. Ambetter plans typically include deductibles that apply to certain healthcare services such as hospital visits, medical procedures, or specialized treatments.
Once the deductible has been met during the coverage year, the insurance plan may begin paying a portion of the remaining healthcare costs according to the plan’s cost-sharing structure. Deductible amounts can vary depending on the specific plan tier selected.
Understanding deductibles can help individuals evaluate how healthcare costs may be distributed throughout the year when using their insurance coverage.
23. What is a copay in an Ambetter health insurance plan?
What is a copay in an Ambetter health insurance plan?
A copay, or copayment, is a fixed amount that a member may pay when receiving certain medical services. Copays commonly apply to services such as doctor visits, urgent care appointments, or prescription medications depending on the structure of the health insurance plan.
The copay amount is usually established by the insurance policy and is paid at the time of the appointment or when the service is received. The insurance company then covers the remaining eligible portion of the cost according to the plan’s coverage terms.
Copays help make healthcare costs more predictable by allowing members to know the approximate cost of certain services before receiving care.
24. What is coinsurance in an Ambetter health insurance plan?
What is coinsurance in an Ambetter health insurance plan?
Coinsurance is a cost-sharing arrangement in which the insurance company and the policyholder share the cost of covered medical services after the deductible has been met. Instead of paying a fixed copay, the patient pays a percentage of the total medical bill.
For example, if a plan includes 20 percent coinsurance, the policyholder may pay 20 percent of the covered service cost while the insurance company covers the remaining 80 percent. Coinsurance continues until the plan’s out-of-pocket maximum has been reached.
Understanding how coinsurance works can help individuals estimate potential healthcare expenses when using medical services.
25. What is the out-of-pocket maximum in an Ambetter plan?
What is the out-of-pocket maximum in an Ambetter plan?
The out-of-pocket maximum is the highest amount a policyholder may be required to pay for covered healthcare services during a plan year. Once this limit is reached, the insurance company generally covers the remaining eligible medical costs for the rest of the coverage period.
Out-of-pocket costs that contribute toward this limit may include deductibles, copays, and coinsurance payments. Premium payments are usually not included in the out-of-pocket maximum calculation.
This limit provides financial protection by ensuring healthcare costs remain manageable even if a member experiences significant medical expenses during the year.
26. Do Ambetter plans include different cost tiers?
Do Ambetter plans include different cost tiers?
Ambetter health insurance plans are commonly offered in different coverage tiers that balance monthly premiums with cost-sharing responsibilities. These tiers allow individuals to choose a plan that aligns with their healthcare usage and financial preferences.
Some plans may offer lower monthly premiums but higher deductibles and cost-sharing requirements, while others may have higher premiums but lower out-of-pocket costs when healthcare services are used.
Comparing plan tiers carefully can help individuals choose coverage that best fits their expected healthcare needs.
27. Can Ambetter plan costs vary by state?
Can Ambetter plan costs vary by state?
Yes, Ambetter health insurance plan costs can vary depending on the state where coverage is offered. Healthcare provider networks, regional medical costs, and state insurance regulations all influence how insurance plans are priced in different areas.
Because of these differences, individuals in one state may see different premium levels, deductibles, or coverage options compared to individuals in another region.
Individuals interested in reviewing coverage options available in their area can explore health insurance plans by state to better understand local coverage availability.
28. Does Ambetter offer financial assistance through the Marketplace?
Does Ambetter offer financial assistance through the Marketplace?
Many Marketplace health insurance plans, including those offered by Ambetter, may qualify for financial assistance programs that help reduce the cost of coverage. These programs are typically based on household income and eligibility guidelines established by Marketplace rules.
Financial assistance may reduce monthly premiums or help lower certain cost-sharing expenses depending on the individual’s eligibility.
Understanding available assistance programs can help individuals determine whether Marketplace coverage may be more affordable for their household.
29. What factors influence the cost of an Ambetter plan?
What factors influence the cost of an Ambetter plan?
Several factors can influence the cost of an Ambetter health insurance plan. These may include the plan tier selected, the geographic region where coverage is offered, the age of the policyholder, and the number of individuals included on the policy.
Healthcare provider networks and regional medical costs also influence insurance pricing because insurers must account for the cost of medical services in different locations.
Comparing plan features carefully can help individuals select coverage that balances monthly premium costs with potential healthcare expenses.
30. Where can someone learn more about Ambetter plan costs?
Where can someone learn more about Ambetter plan costs?
Individuals interested in learning more about Ambetter health insurance costs can review educational resources that explain plan structures, cost-sharing models, and coverage options available through Marketplace plans.
Information about plan features and coverage options can be found by visiting Ambetter health insurance plans. Additional educational resources are also available through the Vivna health insurance blog, which explains how health insurance coverage works.
Understanding insurance costs helps individuals compare plans more effectively and choose coverage that aligns with their healthcare and financial needs.
31. How much do Ambetter doctor visits typically cost?
How much do Ambetter doctor visits typically cost?
The cost of doctor visits under an Ambetter health insurance plan depends on the specific plan tier and cost-sharing structure selected. Many Ambetter plans include copays for primary care visits, which means members pay a fixed amount when seeing their doctor while the insurance plan covers the remaining portion of the visit cost.
Some plans may also apply the deductible before certain services are covered. Once the deductible has been met, copays or coinsurance may apply depending on the type of medical service received. Because each Ambetter plan has its own cost structure, the exact cost of a doctor visit may vary.
Reviewing plan documents and provider network details can help individuals better understand the expected cost of doctor visits before scheduling appointments.
32. How much do specialist visits cost with Ambetter plans?
How much do specialist visits cost with Ambetter plans?
Specialist visits under Ambetter health insurance plans may involve either a copay or coinsurance depending on the specific policy structure. Specialists include physicians who focus on particular areas of medicine such as cardiology, dermatology, orthopedics, or neurology.
Because specialist care often involves advanced expertise and diagnostic services, these visits may have higher copays or coinsurance percentages compared to routine primary care appointments. The exact cost depends on the plan tier and the negotiated pricing agreements within the provider network.
Reviewing provider networks and coverage details before scheduling specialist visits can help members better estimate healthcare costs associated with specialized medical care.
33. How much does urgent care cost with Ambetter insurance?
How much does urgent care cost with Ambetter insurance?
Urgent care visits under Ambetter plans often involve a copay or coinsurance amount depending on the coverage structure of the policy. Urgent care centers treat non-life-threatening conditions such as minor injuries, infections, or illnesses that require prompt medical attention but do not require emergency room care.
Because urgent care facilities operate with fewer resources than hospital emergency departments, the cost of treatment is typically lower than emergency room visits. Health insurance plans often encourage members to use urgent care for appropriate medical situations to help manage healthcare expenses.
Understanding the difference between urgent care and emergency services can help individuals make informed decisions when seeking medical treatment.
34. How much do emergency room visits cost with Ambetter?
How much do emergency room visits cost with Ambetter?
Emergency room visits under Ambetter health insurance plans typically involve higher copays or coinsurance compared to routine medical services. Emergency departments provide immediate care for serious or life-threatening conditions, which requires specialized staff, equipment, and hospital resources.
Because of the complexity of emergency care, the cost of treatment can vary depending on the medical services required during the visit. Insurance coverage helps reduce the overall cost by sharing expenses according to the plan’s deductible and coinsurance structure.
Emergency care is generally covered regardless of whether the hospital is within the provider network, ensuring individuals can receive urgent medical attention when needed.
35. How do prescription drug costs work with Ambetter plans?
How do prescription drug costs work with Ambetter plans?
Prescription drug coverage under Ambetter plans typically follows a formulary system that organizes medications into different pricing tiers. Each tier represents a different cost level depending on whether the medication is generic, brand-name, or a specialty drug.
Lower-tier medications often have lower copays, while higher-tier medications may involve greater coinsurance costs. Pharmacies submit claims to the insurance company when prescriptions are filled, allowing the insurance plan to apply coverage rules based on the medication tier.
Reviewing the prescription drug formulary can help members better understand how medication costs are structured within their insurance plan.
36. What happens when an Ambetter deductible is met?
What happens when an Ambetter deductible is met?
Once the deductible in an Ambetter health insurance plan has been met, the insurance company begins sharing the cost of covered healthcare services according to the policy’s cost-sharing structure. At this point, members may pay copays or coinsurance for services rather than the full cost of treatment.
This cost-sharing arrangement continues until the member reaches the plan’s out-of-pocket maximum. After reaching that limit, the insurance plan typically covers the remaining eligible healthcare costs for the rest of the coverage year.
Understanding how deductibles function within a plan can help individuals estimate potential healthcare expenses throughout the year.
37. How does the out-of-pocket maximum protect Ambetter members?
How does the out-of-pocket maximum protect Ambetter members?
The out-of-pocket maximum provides financial protection by limiting the total amount a member must pay for covered healthcare services during the policy year. Once this limit has been reached, the insurance company typically covers the remaining eligible medical expenses.
This feature is designed to prevent individuals from facing unlimited healthcare costs during serious medical situations. Costs that contribute toward the out-of-pocket maximum may include deductibles, copays, and coinsurance payments.
Understanding how the out-of-pocket maximum works can help individuals better plan for healthcare expenses throughout the coverage year.
38. Why do Ambetter plan costs vary between regions?
Why do Ambetter plan costs vary between regions?
Ambetter health insurance plan costs vary between regions because healthcare pricing, provider networks, and state insurance regulations differ across the country. Medical service costs, hospital pricing structures, and local healthcare systems influence how insurance plans are priced within each state.
Because of these regional differences, the same type of plan may have different premium levels or cost-sharing structures depending on where coverage is offered.
Individuals who want to explore health insurance availability in their location can review health insurance plans by state to better understand coverage options available in their area.
39. How can someone estimate their Ambetter healthcare costs?
How can someone estimate their Ambetter healthcare costs?
Estimating healthcare costs under an Ambetter plan involves reviewing several important plan features, including monthly premiums, deductibles, copays, coinsurance percentages, and the out-of-pocket maximum. These elements work together to determine how healthcare expenses are shared between the policyholder and the insurance company.
Individuals may also consider how often they expect to visit doctors, fill prescriptions, or receive medical services during the year. Understanding these factors can help estimate how much healthcare coverage may cost overall.
Reviewing plan summaries and coverage details carefully can help individuals make informed decisions when selecting a health insurance policy.
40. Where can someone compare Ambetter health insurance plans?
Where can someone compare Ambetter health insurance plans?
Individuals interested in comparing Ambetter health insurance plans can review plan details, provider networks, and coverage options through educational resources that explain how Marketplace coverage works. Comparing plan tiers can help determine which coverage structure best fits individual healthcare needs and budget preferences.
More information about Ambetter plan options and coverage features can be found by visiting Ambetter health insurance plans. Additional educational resources are available through the Vivna health insurance blog, which explains how health insurance coverage works.
Understanding Ambetter Plan Types and Coverage Options
Ambetter health insurance plans are designed to provide comprehensive medical coverage through the Health Insurance Marketplace. These plans typically include a variety of coverage options that allow individuals and families to choose a policy based on their healthcare needs and budget. Ambetter plans generally include essential health benefits such as doctor visits, preventive care, hospital services, prescription medications, and mental health care. Because Marketplace plans are structured in multiple coverage tiers, individuals may select plans with different premium levels and cost-sharing structures. Understanding how Ambetter plans are organized can help individuals compare coverage options more effectively and choose a plan that provides access to the healthcare services they need. More information about available plans can be found by visiting Ambetter health insurance plans.
FAQ's
41. What types of health insurance plans does Ambetter offer?
What types of health insurance plans does Ambetter offer?
Ambetter primarily offers Affordable Care Act Marketplace health insurance plans designed to provide comprehensive medical coverage. These plans are structured to include essential health benefits such as preventive care, doctor visits, hospital treatment, prescription medications, and mental health services.
Ambetter plans are typically organized into different coverage tiers that balance monthly premiums with deductibles, copays, and coinsurance. These plan options allow individuals to choose coverage based on their healthcare needs and financial preferences.
Understanding the differences between plan tiers can help individuals select a policy that aligns with their expected healthcare usage and budget.
42. What are Ambetter plan tiers?
What are Ambetter plan tiers?
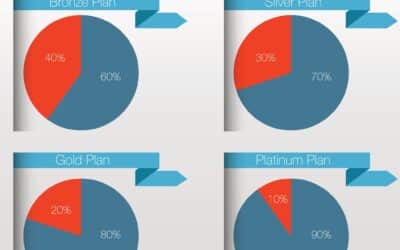
Ambetter health insurance plans are often offered in multiple coverage tiers that help balance monthly premium costs with out-of-pocket healthcare expenses. These tiers are typically categorized in levels that represent different cost-sharing structures.
Plans with lower monthly premiums may include higher deductibles or coinsurance, while plans with higher premiums may reduce the cost of medical services when care is received. This structure allows individuals to select coverage based on their expected healthcare usage.
Comparing plan tiers carefully can help individuals find coverage that provides the best balance between affordability and access to healthcare services.
43. What services are included in Ambetter coverage?
What services are included in Ambetter coverage?
Ambetter health insurance plans typically include a wide range of healthcare services required under Affordable Care Act regulations. These services may include preventive care visits, doctor appointments, hospital treatment, prescription medications, emergency care, and mental health services.
Preventive care services are designed to support long-term wellness by helping detect medical conditions early. Hospital services and physician care help ensure individuals have access to treatment when medical needs arise.
Because coverage details may vary depending on the specific plan selected, reviewing policy documents can help members understand which services are included in their insurance plan.
44. Does Ambetter cover preventive healthcare services?
Does Ambetter cover preventive healthcare services?
Ambetter plans generally include preventive healthcare services that help individuals maintain overall wellness and identify health concerns early. Preventive care may include routine health checkups, screenings, immunizations, and other services recommended by healthcare professionals.
Preventive services are designed to detect potential health issues before they develop into more serious medical conditions. Regular access to preventive care can help individuals manage their health more effectively and support long-term wellbeing.
45. Does Ambetter provide prescription drug coverage?
Does Ambetter provide prescription drug coverage?
Ambetter health insurance plans typically include prescription drug coverage as part of their comprehensive medical benefits. Prescription coverage allows members to obtain medications through pharmacies that participate in the plan’s pharmacy network.
Prescription medications are often categorized into different formulary tiers, which determine the cost-sharing requirements for each medication. Generic medications may have lower copays while brand-name or specialty medications may involve higher coinsurance.
Reviewing the prescription formulary can help members understand how medication costs are structured within their plan.
46. Does Ambetter cover mental health services?
Does Ambetter cover mental health services?
Ambetter health insurance plans generally include coverage for mental health services as part of their essential health benefits. These services may include therapy visits, counseling services, psychiatric care, and treatment for behavioral health conditions.
Mental health coverage helps ensure individuals have access to professional support for emotional wellbeing and behavioral health concerns. Coverage details may vary depending on the specific policy and provider network.
47. Are Ambetter plans available for families?
Are Ambetter plans available for families?
Ambetter health insurance plans are commonly available for individuals as well as families seeking Marketplace health coverage. Family plans allow multiple household members to receive healthcare coverage under a single insurance policy.
Family coverage typically includes access to preventive care, physician services, hospital treatment, and prescription medications for covered household members.
Comparing plan options can help families select coverage that provides access to preferred healthcare providers and medical services.
48. Can individuals compare Ambetter plans before enrolling?
Can individuals compare Ambetter plans before enrolling?
Yes, individuals can compare Ambetter health insurance plans before selecting coverage. Reviewing plan summaries allows consumers to evaluate premiums, deductibles, provider networks, and coverage benefits.
Comparing plan details helps individuals determine which policy best fits their healthcare needs and financial situation. Reviewing coverage options carefully can also help ensure preferred doctors and hospitals are included in the plan’s network.
49. Do Ambetter plans include emergency care coverage?
Do Ambetter plans include emergency care coverage?
Ambetter health insurance plans typically include emergency care coverage for serious medical conditions that require immediate treatment. Emergency services may include hospital emergency room care, ambulance services, and urgent medical procedures necessary to stabilize a patient.
Emergency care is generally covered regardless of whether the hospital is within the plan’s provider network, ensuring individuals can seek urgent treatment when needed.
50. Where can someone learn more about Ambetter coverage options?
Where can someone learn more about Ambetter coverage options?
Individuals who want to learn more about Ambetter health insurance coverage can review plan information that explains provider networks, cost-sharing structures, and available healthcare services. Understanding how coverage works can help individuals make informed decisions when selecting insurance.
More information about available coverage options can be found by visiting Ambetter health insurance plans. Educational resources are also available through the Vivna health insurance blog.
51. Do Ambetter plans cover hospital services?
Do Ambetter plans cover hospital services?
Ambetter health insurance plans generally include coverage for hospital services as part of their comprehensive medical benefits. Hospital coverage may include inpatient treatment, surgeries, diagnostic testing, and other medical procedures that require care within a hospital facility.
Hospital services are typically subject to cost-sharing requirements such as deductibles, copays, or coinsurance depending on the structure of the specific Ambetter plan. Provider networks also play an important role in determining the cost of hospital care.
Receiving treatment at an in-network hospital may help reduce the cost of care because negotiated pricing agreements apply to covered services.
52. Do Ambetter plans cover maternity care?
Do Ambetter plans cover maternity care?
Ambetter health insurance plans typically include maternity and newborn care as part of the essential health benefits required under Affordable Care Act Marketplace coverage. These services may include prenatal visits, labor and delivery services, and postnatal care.
Maternity coverage helps ensure individuals receive appropriate medical support throughout pregnancy and childbirth. Coverage details such as deductibles, copays, or coinsurance may apply depending on the specific policy selected.
Reviewing plan summaries carefully can help individuals understand how maternity services are covered within their health insurance plan.
53. Does Ambetter cover preventive screenings?
Does Ambetter cover preventive screenings?
Ambetter health insurance plans generally include preventive screenings designed to help identify potential health concerns early. Preventive screenings may include services such as blood pressure checks, cholesterol testing, cancer screenings, and other medical evaluations recommended by healthcare professionals.
Preventive healthcare services are intended to help individuals maintain overall wellness and detect medical conditions before they become serious health concerns. Early detection allows healthcare providers to recommend appropriate treatment or lifestyle adjustments.
Regular preventive care is an important part of maintaining long-term health and managing potential medical risks.
54. Does Ambetter health insurance include mental health and behavioral health coverage?
Does Ambetter health insurance include mental health and behavioral health coverage?
Ambetter health insurance plans typically include coverage for mental health and behavioral health services as part of their essential health benefits. These services may include therapy visits, counseling sessions, psychiatric treatment, and other forms of behavioral healthcare.
Mental health coverage helps ensure individuals have access to professional support for emotional wellbeing and behavioral health concerns. Access to mental health services plays an important role in supporting overall health.
Coverage availability and provider networks may vary depending on the specific Ambetter plan and regional healthcare providers.
55. Does Ambetter cover emergency medical services?
Does Ambetter cover emergency medical services?
Ambetter health insurance plans generally include coverage for emergency medical services when individuals require immediate medical attention for serious health conditions. Emergency services may include hospital emergency room treatment, ambulance services, and other urgent medical interventions.
Emergency care is typically covered regardless of whether the hospital is within the provider network because immediate treatment may be required to stabilize a patient’s condition.
Insurance coverage helps reduce the cost of emergency care by sharing expenses according to the plan’s deductible and coinsurance structure.
56. Do Ambetter plans cover prescription medications?
Do Ambetter plans cover prescription medications?
Ambetter health insurance plans generally include prescription medication coverage through participating pharmacy networks. Prescription coverage allows members to obtain medications prescribed by healthcare providers while sharing costs according to the plan’s formulary structure.
Medications are typically organized into tiers that determine cost-sharing requirements. Generic medications may have lower copays, while brand-name or specialty medications may involve higher coinsurance.
Reviewing the prescription drug formulary can help members better understand medication coverage and potential costs.
57. Do Ambetter plans cover specialist care?
Do Ambetter plans cover specialist care?
Ambetter health insurance plans generally include coverage for specialist care when individuals require medical treatment from physicians who focus on specific areas of healthcare. Specialists may include cardiologists, dermatologists, neurologists, orthopedic physicians, and other medical professionals.
Specialist visits may require copays or coinsurance depending on the structure of the specific Ambetter plan. Some plans may also require referrals from primary care physicians before scheduling specialist appointments.
Understanding how specialist care is covered can help members navigate provider networks more effectively.
58. Do Ambetter plans include laboratory and diagnostic testing?
Do Ambetter plans include laboratory and diagnostic testing?
Ambetter health insurance plans generally include coverage for laboratory services and diagnostic testing when these services are medically necessary. Diagnostic services may include blood tests, imaging studies, and other medical tests used to evaluate health conditions.
Healthcare providers may recommend laboratory testing to diagnose illnesses, monitor ongoing medical conditions, or evaluate treatment effectiveness.
Coverage for diagnostic testing may involve deductibles, copays, or coinsurance depending on the specific plan structure.
59. Are preventive wellness visits included in Ambetter plans?
Are preventive wellness visits included in Ambetter plans?
Ambetter health insurance plans typically include preventive wellness visits designed to help individuals maintain overall health. These visits allow healthcare providers to evaluate general health, perform screenings, and discuss lifestyle factors that may influence long-term wellness.
Preventive visits may help detect health concerns early and allow doctors to recommend treatment or lifestyle adjustments when needed.
Regular preventive care can play an important role in maintaining overall health and preventing more serious medical conditions.
60. Where can individuals learn more about Ambetter plan benefits?
Where can individuals learn more about Ambetter plan benefits?
Individuals who want to learn more about Ambetter plan benefits can review plan documentation and educational resources that explain coverage features, provider networks, and cost-sharing structures.
Additional information about Ambetter coverage options can be found by visiting Ambetter health insurance plans. Educational resources such as the Vivna health insurance blog may also provide helpful information about how health insurance coverage works.
Choosing a Dental Insurance Plan
Ambetter health insurance plans are typically available through the Health Insurance Marketplace during designated enrollment periods. Individuals and families who do not receive health coverage through an employer may be able to enroll in Ambetter plans depending on eligibility requirements and state availability. Enrollment opportunities generally occur during the annual open enrollment period, although certain life events may qualify individuals for special enrollment opportunities outside the standard enrollment window. Understanding how eligibility and enrollment timelines work can help individuals determine when they can apply for coverage and select a health insurance plan that meets their healthcare needs. Individuals interested in learning more about enrollment opportunities can review open enrollment health insurance information.
FAQ's
61. When can someone enroll in an Ambetter health insurance plan?
When can someone enroll in an Ambetter health insurance plan?
Ambetter health insurance plans are generally available for enrollment during the annual Health Insurance Marketplace open enrollment period. During this time, individuals and families can review plan options and select coverage for the upcoming coverage year.
Open enrollment typically occurs once each year and allows consumers to compare insurance plans, provider networks, and coverage benefits before choosing a policy. Enrolling during this period ensures that coverage begins according to the Marketplace schedule.
Individuals who want to learn more about enrollment timelines can review open enrollment health insurance information to better understand how Marketplace enrollment works.
62. What is the Health Insurance Marketplace?
What is the Health Insurance Marketplace?
The Health Insurance Marketplace is a platform where individuals and families can compare health insurance plans offered by different insurance companies. Marketplace plans are designed to meet Affordable Care Act standards and provide essential health benefits.
Through the Marketplace, consumers can review available plans, compare coverage features, and determine whether they qualify for financial assistance programs that may help reduce the cost of coverage.
Many Ambetter plans are offered through the Marketplace, allowing individuals to explore coverage options that meet their healthcare needs.
63. Who is eligible to enroll in an Ambetter health insurance plan?
Who is eligible to enroll in an Ambetter health insurance plan?
Eligibility for Ambetter health insurance plans generally includes individuals and families who do not receive employer-sponsored health coverage and who meet Marketplace enrollment requirements. Eligibility guidelines may vary depending on state regulations and individual circumstances.
Individuals may enroll in Marketplace plans if they are residents of a state where Ambetter coverage is offered and meet the eligibility requirements established for Marketplace enrollment.
To explore available coverage options by location, individuals can review health insurance plans by state.
64. Can individuals enroll in Ambetter coverage outside open enrollment?
Can individuals enroll in Ambetter coverage outside open enrollment?
In certain situations, individuals may be able to enroll in Ambetter health insurance outside the standard open enrollment period through a Special Enrollment Period. Special enrollment opportunities may be triggered by qualifying life events.
Qualifying events may include circumstances such as moving to a new state, changes in household size, or loss of other health insurance coverage. These events may allow individuals to apply for coverage during a limited enrollment window.
Understanding special enrollment rules can help individuals determine whether they qualify to enroll outside the regular enrollment period.
65. What is a Special Enrollment Period?
What is a Special Enrollment Period?
A Special Enrollment Period is a limited timeframe that allows individuals to enroll in health insurance coverage outside the annual open enrollment period. Special enrollment is typically triggered by qualifying life events that affect an individual’s healthcare coverage situation.
Examples of qualifying events may include losing existing health insurance coverage, moving to a different state, or experiencing changes in household size.
Special Enrollment Periods help ensure individuals have opportunities to obtain health insurance coverage when significant life changes occur.
66. Can families enroll together in an Ambetter plan?
Can families enroll together in an Ambetter plan?
Yes, Ambetter health insurance plans may allow families to enroll under a single policy. Family coverage enables multiple household members to receive healthcare benefits through one insurance plan.
Family plans may include coverage for preventive care, doctor visits, hospital treatment, and prescription medications for all covered members.
Comparing available plan options carefully can help families select coverage that provides access to the healthcare services they need.
67. Can someone switch to an Ambetter plan from another insurance provider?
Can someone switch to an Ambetter plan from another insurance provider?
Individuals may have the opportunity to switch to an Ambetter health insurance plan during the annual open enrollment period. During this time, consumers can compare coverage options and select a new health insurance plan if they choose to change providers.
Switching plans allows individuals to review different provider networks, coverage features, and cost structures before selecting coverage for the upcoming year.
Reviewing available plan options carefully can help individuals determine whether changing coverage providers meets their healthcare needs.
68. Does income affect eligibility for Marketplace financial assistance?
Does income affect eligibility for Marketplace financial assistance?
Income may influence eligibility for financial assistance programs available through the Health Insurance Marketplace. These programs are designed to help eligible individuals reduce the cost of health insurance coverage.
Eligibility guidelines are based on household income and other factors defined by Marketplace rules. Individuals who qualify may receive assistance that helps lower monthly premiums or reduce certain out-of-pocket costs.
Understanding these assistance programs can help individuals determine whether Marketplace coverage may be more affordable.
69. How can someone prepare to enroll in an Ambetter plan?
How can someone prepare to enroll in an Ambetter plan?
Preparing to enroll in an Ambetter health insurance plan often involves reviewing available coverage options, comparing provider networks, and understanding plan cost structures such as premiums and deductibles.
Individuals may also gather information related to household members, expected healthcare needs, and preferred medical providers before selecting a plan.
Taking time to compare coverage details carefully can help individuals choose a plan that provides access to the healthcare services they expect to use.
70. Where can someone learn more about Ambetter enrollment?
Where can someone learn more about Ambetter enrollment?
Individuals interested in learning more about Ambetter enrollment opportunities can review educational resources that explain Marketplace enrollment timelines, plan options, and coverage features.
Additional information about Ambetter coverage and plan availability can be found by visiting Ambetter health insurance plans. Individuals may also review helpful articles through the Vivna health insurance blog.
71. What documents may be needed to enroll in an Ambetter plan?
What documents may be needed to enroll in an Ambetter plan?
When enrolling in an Ambetter health insurance plan through the Health Insurance Marketplace, individuals may need to provide certain information to complete the enrollment process. This information may include personal identification details, household information, and income documentation used to determine eligibility for coverage or financial assistance programs.
Providing accurate information helps ensure that Marketplace applications are processed correctly and that individuals are matched with the appropriate coverage options available in their region.
Reviewing enrollment guidelines carefully can help individuals prepare the necessary information before beginning the application process.
72. Can someone enroll in Ambetter coverage for the first time through the Marketplace?
Can someone enroll in Ambetter coverage for the first time through the Marketplace?
Yes, individuals who have not previously had Ambetter health insurance may enroll in coverage through the Health Insurance Marketplace if they meet eligibility requirements. Marketplace enrollment allows individuals to compare available insurance plans and select coverage that fits their healthcare needs.
Because Ambetter plans are offered in many states through Marketplace exchanges, individuals may be able to review multiple plan options depending on where they live.
Understanding Marketplace enrollment periods can help individuals determine when they can apply for coverage.
73. Can someone renew their Ambetter health insurance each year?
Can someone renew their Ambetter health insurance each year?
Ambetter health insurance plans are typically renewed annually during the Health Insurance Marketplace open enrollment period. During this time, individuals may review their current coverage and decide whether to continue with the same plan or select a different policy for the upcoming coverage year.
Renewal provides an opportunity to review any changes in provider networks, premiums, or plan benefits before confirming coverage for the next policy year.
Carefully reviewing plan details during the renewal period helps ensure that the selected coverage continues to meet healthcare needs.
74. Can someone change their Ambetter plan during open enrollment?
Can someone change their Ambetter plan during open enrollment?
Yes, individuals typically have the opportunity to change their Ambetter health insurance plan during the annual open enrollment period. Open enrollment allows consumers to compare plan options and select coverage that better fits their healthcare needs.
During this period, individuals may review differences in premiums, deductibles, provider networks, and coverage benefits when deciding whether to keep their current plan or choose a new option.
Comparing plan options carefully during open enrollment can help individuals ensure their insurance coverage aligns with their healthcare preferences.
75. What happens after someone enrolls in an Ambetter plan?
What happens after someone enrolls in an Ambetter plan?
After enrolling in an Ambetter health insurance plan, members typically receive confirmation of coverage along with plan information that explains how their benefits work. This information may include an insurance identification card, provider network details, and instructions on how to access covered healthcare services.
Members can then begin scheduling medical appointments with participating healthcare providers according to the plan’s network guidelines.
Understanding how to use insurance benefits helps individuals access healthcare services more efficiently after enrollment.
76. Can individuals enroll in Ambetter if they recently moved to a new state?
Can individuals enroll in Ambetter if they recently moved to a new state?
Moving to a new state may qualify individuals for a Special Enrollment Period, which can allow them to enroll in health insurance coverage outside the standard open enrollment period. Relocation may change the insurance plans and provider networks available to an individual.
When individuals move to a different state, they may need to review the health insurance plans available in their new location and select coverage that includes local healthcare providers.
Individuals can review health insurance plans available by state to better understand which coverage options may be offered where they live.
77. Can someone enroll in Ambetter if they lose other health insurance coverage?
Can someone enroll in Ambetter if they lose other health insurance coverage?
Losing existing health insurance coverage may qualify an individual for a Special Enrollment Period. This type of enrollment opportunity allows individuals to apply for Marketplace coverage outside the standard open enrollment window.
Coverage loss may occur when employer-sponsored insurance ends, when an individual ages out of a family plan, or when other qualifying coverage changes occur.
Special enrollment opportunities help ensure individuals can obtain health insurance coverage when their previous insurance ends.
78. Can someone enroll in Ambetter coverage after getting married or having a child?
Can someone enroll in Ambetter coverage after getting married or having a child?
Certain life events such as marriage or the birth of a child may qualify individuals for a Special Enrollment Period through the Health Insurance Marketplace. These life changes may allow individuals to enroll in coverage or modify an existing policy outside the annual open enrollment period.
Special enrollment helps ensure families can update their health insurance coverage when household circumstances change.
Reviewing enrollment rules carefully can help individuals determine whether they qualify for special enrollment opportunities.
79. Can someone enroll in Ambetter coverage if they become self-employed?
Can someone enroll in Ambetter coverage if they become self-employed?
Individuals who become self-employed may explore health insurance coverage options available through the Health Insurance Marketplace. Marketplace plans such as Ambetter may provide coverage options for individuals who do not receive employer-sponsored health insurance.
Self-employed individuals can compare available plans, provider networks, and coverage benefits to determine which policy best fits their healthcare needs.
Understanding Marketplace coverage options can help self-employed individuals maintain consistent access to healthcare services.
80. Where can someone find more information about Ambetter eligibility and enrollment?
Where can someone find more information about Ambetter eligibility and enrollment?
Individuals interested in learning more about Ambetter eligibility and enrollment options can review educational resources that explain Marketplace coverage, plan availability, and enrollment timelines.
More information about coverage options can be found by visiting Ambetter health insurance plans. Additional insights about health insurance coverage are also available through the Vivna health insurance blog.
Understanding How to Use Ambetter Health Insurance
Once enrolled in an Ambetter health insurance plan, members can begin using their coverage to access healthcare services within the plan’s provider network. Ambetter plans typically include networks of doctors, hospitals, clinics, pharmacies, and healthcare specialists that work together to provide medical care to members. Understanding how to choose providers, schedule appointments, review insurance claims, and manage healthcare costs can help individuals use their coverage more effectively. Learning how the insurance process works allows members to access healthcare services with greater confidence while managing out-of-pocket costs. Individuals interested in learning more about available plan options and provider networks can explore Ambetter health insurance plans.
FAQ's
81. How do members find doctors that accept Ambetter insurance?
How do members find doctors that accept Ambetter insurance?
Members enrolled in an Ambetter health insurance plan can locate participating healthcare providers by reviewing the plan’s provider network. Provider networks include doctors, hospitals, specialists, and clinics that have agreements with the insurance company to provide services to plan members.
Choosing healthcare providers within the network can help reduce the cost of medical services because negotiated pricing agreements apply to covered treatments. These agreements allow members to access care at lower rates compared to services provided outside the network.
Reviewing provider directories before scheduling appointments can help ensure that a doctor or healthcare facility participates in the Ambetter network.
82. Do members need a primary care doctor with Ambetter plans?
Do members need a primary care doctor with Ambetter plans?
Many health insurance plans encourage members to select a primary care physician who helps coordinate routine healthcare services. A primary care doctor often serves as the first point of contact for general medical concerns, preventive care visits, and ongoing health management.
Primary care physicians may also provide referrals to medical specialists when advanced treatment is required. This coordinated approach helps ensure that members receive appropriate care based on their healthcare needs.
Understanding how primary care physicians support healthcare management can help members navigate their insurance coverage more effectively.
83. How do members schedule appointments using Ambetter insurance?
How do members schedule appointments using Ambetter insurance?
Members typically schedule medical appointments directly with healthcare providers that participate in the Ambetter provider network. When scheduling appointments, members may provide their insurance identification information so the provider can verify coverage.
During the visit, the healthcare provider submits claims to the insurance company for covered services. The insurance company then processes the claim and determines how costs are shared between the insurer and the member according to the plan’s cost-sharing rules.
Understanding how appointments and insurance claims work together can help members access care more efficiently.
84. What is an insurance claim?
What is an insurance claim?
An insurance claim is a request submitted by a healthcare provider to the insurance company for payment of medical services. When members receive treatment, the provider sends details of the services performed to the insurance company for review.
The insurance company evaluates the claim to determine how the cost of the service will be shared according to the member’s policy. After processing the claim, the insurer may pay a portion of the cost while the member may be responsible for deductibles, copays, or coinsurance.
This process allows healthcare providers and insurance companies to coordinate payment for covered medical services.
85. What is an explanation of benefits (EOB)?
What is an explanation of benefits (EOB)?
An Explanation of Benefits, often referred to as an EOB, is a document provided by the insurance company after a medical claim has been processed. The EOB outlines the healthcare services received, the amount billed by the provider, and how the insurance plan applied coverage to those services.
The document also shows how much the insurance company paid and what portion of the cost may be the responsibility of the member. Reviewing the EOB helps members understand how their insurance coverage was applied to the medical service.
Understanding EOB statements can help individuals track healthcare costs and confirm that insurance claims were processed correctly.
86. How do members use their Ambetter insurance card?
How do members use their Ambetter insurance card?
After enrolling in an Ambetter health insurance plan, members typically receive an insurance identification card that contains important information about their coverage. This card is presented when visiting doctors, hospitals, pharmacies, or other healthcare providers.
The information on the card allows healthcare providers to verify coverage and submit claims to the insurance company for covered services. Keeping the insurance card available during medical visits helps ensure healthcare providers can process insurance claims accurately.
87. Do members need referrals to see specialists?
Do members need referrals to see specialists?
Some health insurance plans encourage or require referrals from a primary care physician before members visit certain medical specialists. Referral requirements help coordinate healthcare services and ensure that patients receive the appropriate level of medical care.
The referral process allows primary care physicians to guide patients toward specialists who can address specific medical concerns.
Referral requirements may vary depending on the structure of the specific Ambetter plan and the provider network associated with that coverage.
88. How do members fill prescriptions with Ambetter insurance?
How do members fill prescriptions with Ambetter insurance?
Members can fill prescriptions at pharmacies that participate in the Ambetter pharmacy network. When a prescription is presented at the pharmacy, the pharmacist submits the claim to the insurance company to determine the member’s cost-sharing responsibility.
The insurance plan then applies coverage rules based on the medication tier within the prescription drug formulary. Generic medications may have lower copays, while specialty medications may involve higher coinsurance.
Using pharmacies within the insurance network helps ensure prescription coverage is applied correctly.
89. What should members do if they receive a medical bill?
What should members do if they receive a medical bill?
If members receive a medical bill, they may review the Explanation of Benefits provided by their insurance company to understand how the claim was processed. The EOB shows how much the insurance company paid and what portion of the bill may remain the member’s responsibility.
If there are questions about a medical bill, members may contact the healthcare provider or the insurance company to clarify the charges and confirm that the claim was processed correctly.
Understanding how insurance billing works can help members manage healthcare expenses more effectively.
90. Where can members learn more about using Ambetter coverage?
Where can members learn more about using Ambetter coverage?
Members who want to learn more about how Ambetter health insurance works can review educational resources that explain coverage features, provider networks, and healthcare services available through the plan.
Additional information about coverage options and plan details can be found by visiting Ambetter health insurance plans. Members can also explore helpful educational articles through the Vivna health insurance blog.
91. What should members do if their doctor is not in the Ambetter network?
What should members do if their doctor is not in the Ambetter network?
If a preferred doctor does not participate in the Ambetter provider network, members may consider selecting a different provider who is included in the network. Provider networks include physicians and healthcare facilities that have agreements with the insurance company to deliver covered services at negotiated rates.
Receiving care from in-network providers typically results in lower healthcare costs because the insurance plan applies negotiated pricing to those services. Members may review provider directories to identify participating doctors and healthcare facilities.
Understanding provider networks can help members select healthcare providers that work with their insurance coverage.
92. Can members receive healthcare services outside their Ambetter network?
Can members receive healthcare services outside their Ambetter network?
Some health insurance plans may allow members to receive medical services outside the provider network, although the cost of care may be higher in those situations. Out-of-network providers may not have negotiated pricing agreements with the insurance company.
When services are provided outside the network, members may be responsible for a larger portion of the healthcare cost. Because provider networks vary depending on the specific plan, reviewing network guidelines can help members understand their coverage options.
Using in-network healthcare providers whenever possible can help reduce out-of-pocket healthcare expenses.
93. How do members track their healthcare spending with Ambetter?
How do members track their healthcare spending with Ambetter?
Members can track healthcare spending by reviewing Explanation of Benefits documents and monitoring how deductibles, copays, and coinsurance apply to medical services. These documents provide details about healthcare charges and how insurance coverage was applied to those services.
Tracking healthcare spending helps members understand how close they are to meeting their deductible or reaching their out-of-pocket maximum for the coverage year.
Monitoring healthcare expenses can help individuals better plan for medical costs and understand how their insurance benefits are being used.
94. What should members do if they have questions about their Ambetter coverage?
What should members do if they have questions about their Ambetter coverage?
If members have questions about their Ambetter health insurance coverage, they may review their policy documents or contact their insurance provider for clarification about benefits, provider networks, and cost-sharing structures.
Understanding plan details such as deductibles, copays, and covered services can help members navigate their healthcare coverage more effectively.
Educational resources such as the Vivna health insurance blog may also help explain how different health insurance features work.
95. How can members verify if a medical service is covered?
How can members verify if a medical service is covered?
Members may review their health insurance policy documents or contact their insurance provider to confirm whether a specific medical service is covered under their Ambetter plan. Coverage details depend on the structure of the policy and the provider network associated with that plan.
Healthcare providers may also verify insurance coverage before scheduling procedures or treatments to help ensure services are processed according to the plan’s coverage guidelines.
Confirming coverage in advance can help members better understand potential healthcare costs before receiving treatment.
96. What happens if a member reaches their out-of-pocket maximum?
What happens if a member reaches their out-of-pocket maximum?
Once a member reaches the out-of-pocket maximum for their Ambetter health insurance plan, the insurance company typically covers the remaining eligible healthcare costs for covered services during that plan year.
The out-of-pocket maximum includes certain healthcare expenses such as deductibles, copays, and coinsurance payments. Once this limit has been reached, additional covered medical services may be paid by the insurance plan according to policy guidelines.
This limit helps protect members from extremely high healthcare expenses during a coverage year.
97. How do members keep their Ambetter coverage active?
How do members keep their Ambetter coverage active?
Maintaining active health insurance coverage generally involves keeping policy information up to date and following the requirements established by the insurance plan. Coverage typically remains active as long as the policy remains in good standing according to plan guidelines.
Members may review their policy information regularly to ensure that personal details and coverage information remain accurate throughout the policy year.
Understanding policy guidelines can help members maintain continuous access to healthcare services.
98. Can members update their personal information on their Ambetter plan?
Can members update their personal information on their Ambetter plan?
Members may update certain personal information related to their health insurance coverage if changes occur during the coverage period. Updates may include changes to household information, address details, or other information related to the insurance policy.
Keeping personal information current helps ensure that insurance records remain accurate and that members continue to receive important coverage information.
Accurate information also helps ensure that healthcare claims are processed correctly when medical services are received.
99. How does Ambetter help members access healthcare providers?
How does Ambetter help members access healthcare providers?
Ambetter health insurance plans connect members with provider networks that include doctors, hospitals, clinics, and medical specialists. These networks help coordinate healthcare services and provide access to medical care within the insurance plan’s coverage guidelines.
Provider networks also help manage healthcare costs by establishing negotiated pricing agreements between healthcare providers and the insurance company.
Understanding how provider networks operate can help members select healthcare providers who participate in their insurance plan.
100. Where can individuals learn more about Ambetter health insurance?
Where can individuals learn more about Ambetter health insurance?
Individuals who want to learn more about Ambetter health insurance plans can explore educational resources that explain coverage features, provider networks, and plan benefits. Understanding how insurance coverage works can help individuals make informed decisions when selecting healthcare plans.
More information about coverage options and provider networks can be found by visiting Ambetter health insurance plans. Individuals may also explore additional educational articles through the Vivna health insurance blog.
Reviewing reliable information helps individuals better understand their insurance coverage and healthcare options.
Related Insurance Questions
What is the difference between dental insurance and health insurance?
<p>Dental insurance and health insurance both help manage healthcare costs, but they focus on different types of medical services. Dental insurance is designed specifically to cover services related to oral health, including preventive care such as dental exams, cleanings, and diagnostic imaging. It may also provide coverage for restorative procedures like fillings, crowns, and extractions depending on the plan.</p>
<p>Health insurance, on the other hand, focuses on medical services related to overall physical health. Health insurance plans typically cover doctor visits, hospital care, prescription medications, and medical procedures that treat illnesses or injuries. While both types of insurance help reduce healthcare expenses, they serve different roles in a person’s overall healthcare coverage.</p>
<p>Some dental procedures may overlap with medical coverage if the treatment is related to a medical condition or injury. However, most routine dental care is handled through dental insurance rather than traditional medical plans.</p>
<p>Individuals interested in learning more about medical coverage structures can explore the <a href=”https://vivna.net/vivna-faq-page/health-insurance-faqs/” style=”color:blue; text-decoration:underline;”>Health Insurance FAQs</a> for additional explanations about healthcare coverage options.</p>
<p>For additional educational articles about insurance topics and preventive healthcare, visit the <a href=”https://vivna.net/health-insurance-blog/” style=”color:blue; text-decoration:underline;”>Health Insurance Blog</a>.</p>
How can different types of insurance coverage work together?
Different types of insurance coverage often work together to provide a more complete healthcare protection strategy. Health insurance typically serves as the primary form of coverage, helping pay for doctor visits, hospital care, and medical treatments related to illness or injury. Additional insurance policies may provide benefits for specific healthcare needs.
Dental insurance focuses on oral health services, while vision insurance supports eye care and vision correction. Supplemental insurance plans can provide additional financial assistance when certain medical events occur. By combining multiple types of coverage, individuals may reduce the financial impact of healthcare expenses across different areas of care.
Understanding how these policies work together allows individuals to build a more comprehensive insurance strategy that supports both preventive care and unexpected medical needs.
For additional information about medical coverage structures, visit the Health Insurance FAQs. You can also explore the Supplemental Insurance FAQs for more details about additional coverage options.
How does vision insurance work and what services does it cover?
Vision insurance helps cover services related to eye health and vision correction. These plans are designed to support routine eye exams, diagnostic testing, and vision correction options such as eyeglasses or contact lenses. Regular eye exams help detect vision changes and identify potential eye health concerns early.
Vision insurance plans typically provide coverage for preventive eye exams and may include allowances for eyewear such as lenses or frames. Coverage structures vary depending on the plan, and benefits may include discounts or partial reimbursement for vision correction products.
Maintaining routine eye exams is an important part of preventive healthcare because eye exams can detect vision changes and certain health conditions that may affect eye health. Vision insurance helps make these services more accessible and encourages regular eye care.
Individuals interested in learning more about vision coverage can explore the Vision Insurance FAQs for additional explanations about how vision insurance plans work.
What is supplemental insurance and how does it work?
Supplemental insurance is a type of coverage designed to provide additional financial protection beyond what traditional health insurance policies offer. While health insurance typically covers many medical services, patients may still be responsible for deductibles, copayments, and other out-of-pocket costs. Supplemental insurance helps reduce these financial burdens by providing additional benefits when certain medical events occur.
Examples of supplemental insurance policies may include accident coverage, critical illness coverage, hospital indemnity plans, or other types of protection designed to help offset healthcare expenses. These plans do not replace primary medical insurance but instead provide additional financial support when covered situations arise.
Many individuals choose supplemental coverage to help manage unexpected healthcare costs that may not be fully covered by their primary insurance policy. Understanding how these policies work can help individuals build a more comprehensive healthcare protection strategy.
For more detailed information about supplemental coverage, visit the Supplemental Insurance FAQs page.
Why do some people choose both dental and vision insurance coverage?
Many individuals choose to carry both dental and vision insurance because these plans support preventive healthcare in two important areas of overall wellness. Dental insurance focuses on maintaining oral health through preventive dental visits and restorative procedures when necessary. Vision insurance supports eye health through routine eye exams and vision correction services.
Regular dental and vision checkups allow healthcare professionals to monitor changes in oral and eye health over time. Preventive visits help detect potential concerns early, which can reduce the likelihood of more complex treatments later.
Combining dental and vision insurance coverage can provide broader preventive healthcare support while helping individuals manage the cost of routine services in both areas. Many people include these coverages as part of a larger healthcare planning strategy.
For more information about eye care coverage, visit the Vision Insurance FAQs. For broader healthcare planning resources, individuals may also explore the Health Insurance Blog.
Vivna’s Health Insurance Blog
Our Vivna Insurance blog is designed to help you better understand health insurance, supplemental coverage, dental and vision plans, and life insurance. Through clear, educational articles, we break down complex topics so individuals, families, and business owners can make confident decisions about their coverage and financial protection. Explore our articles below to learn more about how insurance works and how the right coverage can support your long-term health and financial well-being.
Income Based Health Insurance Options Explained | Vivna Insurance
Learn how income affects health insurance options, monthly premiums, subsidy eligibility, and plan comparisons.
Health Coverage Decision Guide | Plans Doctors and Cost Strategy
Health Coverage Decision Guide explains how to choose the right insurance plan doctor and cost strategy based on your healthcare needs.
Lower Health Insurance Costs | Save Using Networks and Plan Strategy
Lower Health Insurance Costs by using smarter network choices, balancing premiums and deductibles, and selecting the right plan for your needs.
Premium vs Deductible Strategy | Choose the Right Plan
Premium vs Deductible Strategy explains how monthly premiums and deductibles work together so you can choose a health plan that fits your budget and expected care needs.
Health Insurance Network Costs | Premiums & Deductibles Guide
Health Insurance Network Costs affect your premiums, deductibles, and provider access. Learn how network size can change what you pay and how to choose the right plan.
Types of Health Plans Explained | HMO, PPO, EPO, and POS
Learn the main types of health plans including HMO, PPO, EPO, and POS. Compare costs, referrals, provider access, and flexibility to choose the right coverage.
EPO vs POS Plans: Key Differences Explained
Learn the differences between EPO vs POS plans including cost, referrals, and provider flexibility to choose the right coverage.
HMO vs PPO Plans: Key Differences Explained
Learn the key differences between HMO vs PPO plans, including costs, flexibility, and provider networks to choose the best coverage.
Ambetter Provider Network | In-Network Rules Explained
Learn how the Ambetter Provider Network works, how to verify doctors, and how in-network rules affect costs.
Ambetter Plan Types | Bronze, Silver & Gold Explained
Learn how Ambetter Plan Types work, compare Bronze, Silver, and Gold tiers, and understand total coverage costs.
Key Factors in Choosing Health Dental and Vision Insurance
Learn key factors in choosing health dental and vision insurance, including costs, provider networks, and coverage benefits.
Affordable Health Insurance Provider | Coverage Guide & Plan Comparison
Learn how to evaluate an Affordable Health Insurance Provider, compare coverage types, and choose plans that protect your health and budget.
Health Insurance Claim Timeline | How Long Claims Take
Learn the Health Insurance Claim Timeline so you know how long claims take and what causes delays.
Health Insurance Claim Appeals | How to Challenge Denials
Learn how Health Insurance Claim Appeals work so you can challenge denied claims, provide documentation, and improve approval chances.
Health Insurance Claim Status | What Happens After Filing
Learn what Health Insurance Claim Status updates mean after filing and how to move a pending claim forward faster.
Health Insurance Claims Process | Step-By-Step Guide
Understand the Health Insurance Claims Process step by step so you can manage medical bills and avoid payment surprises.
Understanding Health Insurance Coverage | What Plans Include and How Benefits Work
A detailed guide to understanding health insurance coverage, including covered services, networks, exclusions, and cost-related rules.
Health Insurance Cost Breakdown Guide
A detailed guide explaining health insurance costs, including premiums, deductibles, copays, coinsurance, and out-of-pocket maximums.
Understanding Health Insurance Enrollment
A detailed guide explaining health insurance enrollment, including timing, eligibility, and how to avoid coverage gaps.
Understanding Health Insurance Basics
A clear guide to understanding health insurance basics, including coverage structure, enrollment rules, and plan selection.
How Health Insurance Costs Change After Major Life Events
Health insurance cost changes often happen after major life events such as marriage, job changes, or relocation.
Vivna Insurance
If you have questions about insurance coverage or need help reviewing your options, the team at Vivna Insurance is here to help. Call 888-730-6001 to speak with a licensed agent and receive guidance tailored to your needs.
Still Have Questions
Located In
Deerfield Beach, Florida